Elon Musk is famous for being one of the wealthiest people in the world. He’s also famous for his tax avoidance. He recently sold out his California interests and home and moved to Texas just so he could avoid paying taxes in California.
“Musk is not exactly gracious in victory. He recently harassed (on Twitter, of course) the head of the United Nations food program, after the official suggested that billionaires devote some of their resources toward ending worldwide hunger. When Wyden posted that whether billionaires should pay taxes isn’t policy that should be determined by a Twitter poll, Musk’s vulgar response was so inappropriate The Post won’t print it and I won’t link to it here.”
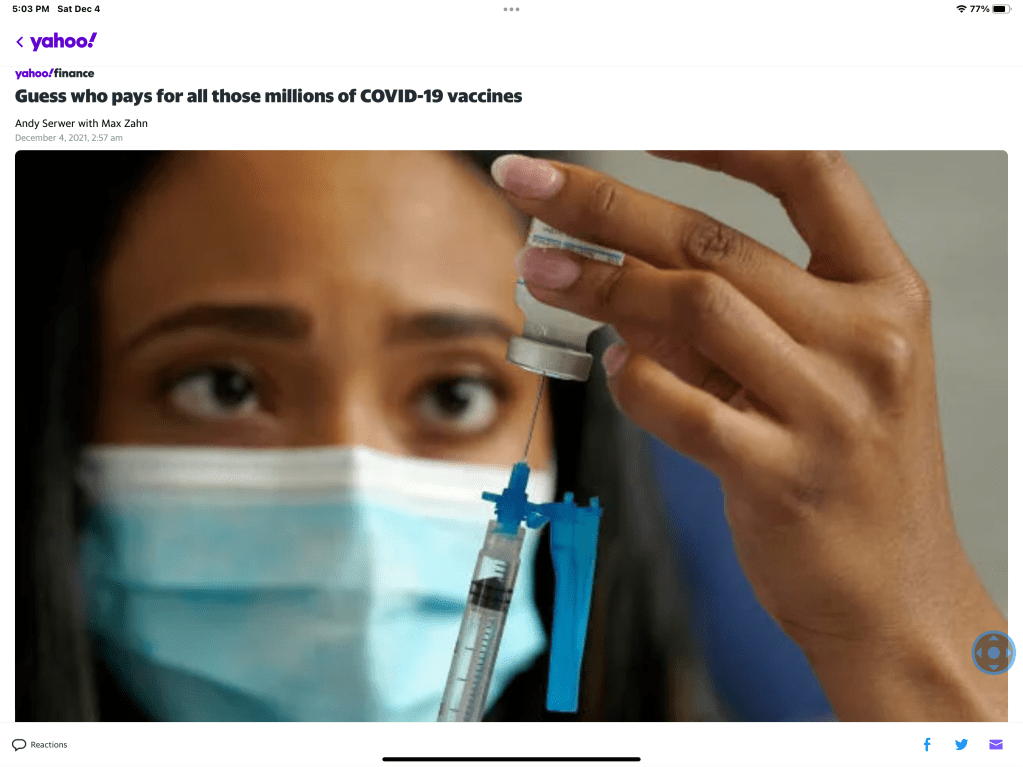
So it comes as no surprise that as we consider who is paying for the COVID vaccine and the hospitalizations of COVID paitents that Elon has not stepped up to help pay for this burden. Just you and me folks.